This neurodevelopmental disorder is diagnosed in children with behavioral symptoms (inattentiveness, hyperactivity, and impulsivity) that are inconsistent with their age.
What is it?
This is a condition that makes it difficult for a child to sit still and concentrate, and it is usually noticeable before the age of six. The effects of ADHD can persist into adolescence and adulthood. Adults may also be diagnosed with the preexisting condition, when persistent problems in higher education, employment, and relationships reveal it. However, the symptoms may not be as clear as they are in children (right). The level of hyperactivity decreases in adults with ADHD, but they struggle more with paying attention, impulsive behavior, and restlessness. The evidence for what causes ADHD is inconclusive,
but it is thought to include a combination of factors. Genetics may play a part, which explains why it runs in families. Observations of brain scans also indicate differences in brain structure, and have identified unusual levels of the neurotransmitters dopamine and norepinephrine . Other possible risk factors include premature birth, low birthweight, and exposure to environmental hazards. The condition is more common in people with learning difficulties. Children with ADHD may also display signs of other conditions such as ASD , tic disorders or Tourette’s , depression , and sleep disorders . Surveys have shown that worldwide this condition affects more than twice as many boys as girls.
Identifying ADHD
A GP cannot officially diagnose ADHD, but if they suspect a child has the disorder they refer them for specialist assessment. The child’s patterns of hyperactivity, inattention, and impulsive behavior are observed over a six-month period before a treatment plan is prepared.
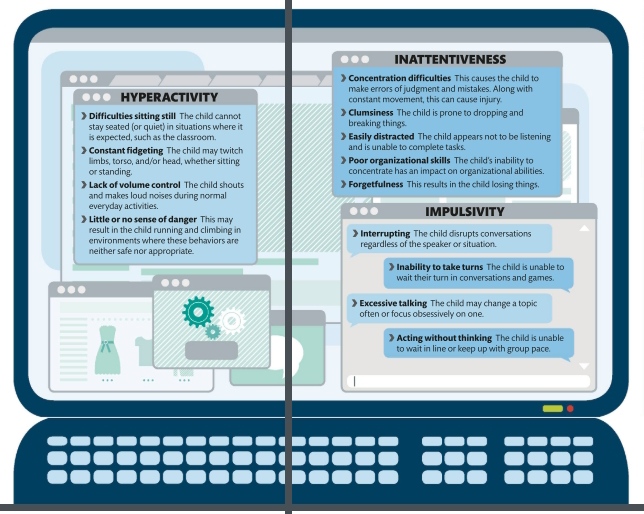
HYPERACTIVITY
❯ Difficulties sitting still The child cannot stay seated (or quiet) in situations where it is expected, such as the classroom.
❯ Constant fidgeting The child may twitch limbs, torso, and/or head, whether sitting or standing.
❯ Lack of volume control The child shouts and makes loud noises during normal everyday activities.
❯ Little or no sense of danger This may result in the child running and climbing in environments where these behaviors are neither safe nor appropriate.
INATTENTIVENESS
❯ Concentration difficulties This causes the child to make errors of judgment and mistakes. Along with constant movement, this can cause injury.
❯ Clumsiness The child is prone to dropping and breaking things.
❯ Easily distracted The child appears not to be listening and is unable to complete tasks.
❯ Poor organizational skills The child’s inability to concentrate has an impact on organizational abilities.
❯ Forgetfulness This results in the child losing things.
IMPULSIVITY
❯ Interrupting The child disrupts conversations regardless of the speaker or situation.
❯ Inability to take turns The child is unable to wait their turn in conversations and games.
❯ Excessive talking The child may change a topic often or focus obsessively on one.
❯ Acting without thinking The child is unable to wait in line or keep up with group pace.
MANAGING ADHD
There are a number of ways that parents can help their child to handle the condition.
❯ Create predictable routines to calm an ADHD sufferer. Schedule daily activities and keep them consistent. Make sure school timetables are clearly set, too.
❯ Set clear boundaries and make sure the child knows what is expected of them; praise positive behavior right away.
❯ Give clear instructions, either visual or verbal, whichever the child finds easier to follow.
❯ Use an incentive scheme, for example, have a star/points chart whereby a child can earn privileges for good behavior.
TREATMENT
❯ Behavioral therapies to help the child and their family manage day to day; psychoeducation for families and caregivers.
❯ Lifestyle management such as improving physical health and reducing stress to calm the child.
❯ Medication can calm (not cure) the person so that they are less impulsive and hyperactive. Stimulants increase dopamine levels and trigger the area of the brain involved in concentration.
“… an ADHD brain [is] like a browser with way too
Pat Noue, ADHD Collective
many open tabs.”
